Nerve pain (neuropathic pain)
Learn about nerve (neuropathic) pain in MS. Explore what it feels like, why it happens and the drug treatments, therapies and self-management approaches that can help.
Trigeminal neuralgia is a type of nerve pain that affects the face, usually down one side. It can cause stabbing, shooting or burning sensations in your forehead, temple, cheek and jaw. This facial pain can be very intense and happen suddenly. The pain may last a few seconds or minutes but may repeat many times during an attack. For some people, the face pain is present all the time.
This page covers what trigeminal neuralgia may feel like, what causes it and treatment options to reduce its impact on your life.
Trigeminal neuralgia, sometimes called tic douloureux, is a type of neuropathic pain in the side of the face. It can be a condition on its own, but sometimes it's a symptom of multiple sclerosis.
The pain is usually on one side of the face (unilateral). In rare cases it happens on both sides of the face (bilateral) but not at the same time.
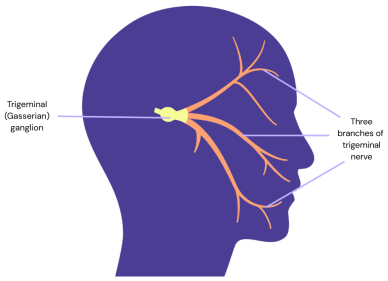
It’s called trigeminal neuralgia because it is the trigeminal nerve which is affected. Neuralgia means pain that follows the path of a nerve. The trigeminal nerve controls the muscles needed for chewing, but it is mainly responsible for the feelings of touch, temperature and pain in the face. There are two trigeminal nerves – one on each side of the face. Each nerve has three main branches, giving the name trigeminal ("tri" meaning three). Trigeminal neuralgia can affect one or more of these branches. The location of your pain depends on which one(s) are affected.
Different people experience trigeminal neuralgia in different ways. It is most commonly felt in the cheek or in the upper or lower jaw, but some people experience pain up towards the eye, ear and forehead, or inside the mouth. It can feel like it is coming from one or more teeth so many people visit their dentist to begin with.
The pain of trigeminal neuralgia is usually felt in two ways.
Attacks can occur many times a day. Some people are aware that an attack is coming, but for most people it arrives unexpectedly. The pain may wake people up at night during sleep, but this is not very common.
For the majority of people with trigeminal neuralgia, facial pain attacks continue for days or months before the pain reduces and goes away. These pain free times are known as periods of remission which can last for months or even years.
Less often, the condition worsens with longer periods of pain that happen more often with no clear remission periods. Pain that's been present for more than three months is described as chronic or persistent pain.
Trigeminal neuralgia has two main causes.
Read more about how damaged nerves can cause pain.
Other causes of secondary trigeminal neuralgia include cysts and tumours.
In some cases, no obvious cause can be found. This is labelled idiopathic trigeminal neuralgia.
Facial pain in MS isn't always trigeminal neuralgia. It can have other causes, such as dental issues, jaw problems, ear infection, headache and post-herpetic neuralgia (a type of nerve pain caused by shingles). These other possible diagnoses may need to be ruled out before MS can be confirmed as the cause. This may involve seeing a dentist and your GP for further investigations.
Research suggests that around three in every 100 people with MS experience trigeminal neuralgia. This is more common than in the general population where it's considered rare. People with MS are estimated to be 15 times more likely to experience this intense facial pain than the general population.
Women are more likely to be affected, as well as people between the ages of 50 and 60. Trigeminal neuralgia rarely affects people under 40 who do not have MS.
If you're under 40 and you have MS, it is particularly important to consider if the facial pain is a symptom of your MS.
Trigeminal neuralgia isn't usually one of the early symptoms in MS. But it is more likely to occur the longer you’ve had MS.
There is no specific test for trigeminal neuralgia. Diagnosis and treatment are based on your description of your pain.
You may have an MRI scan of the brain to rule out other conditions. An MRI would also show if your MS is more active at the moment.
An MRI scan of the trigeminal nerves may be needed to work out what type of trigeminal neuralgia you have. A scan can show if a blood vessel is significantly pressing on the nerve inside the skull and changing its shape (classical trigeminal neuralgia).
If you see your dentist to rule out dental issues as the cause of your facial pain, they may do an X-ray to look for any signs of infection or damage to your teeth.
Trigeminal neuralgia is often triggered by everyday activities which can be difficult to avoid. These can include:
Attacks can also be triggered by things in your external environment, such as:
Less often, the pain can happen unexpectedly with no obvious trigger.
Research has suggested that fampridine may make trigeminal neuralgia worse and possibly trigger this type of pain in someone who is already experiencing altered sensations in the face. Fampridine is taken by some people with MS to improve walking.
If you can identify what sets off your facial pain, you can take steps to avoid or reduce those triggers.
You may find it useful to keep a symptom diary to keep track of your triggers and see if there is any pattern to your attacks.
If you're concerned about your facial pain, and suspect it could be trigeminal neuralgia, you can contact your MS team directly or ask your GP to refer you for an assessment. Try to describe your pain as clearly as possible and say how much it’s affecting you so that you’re referred as quickly as possible.
You may want to keep a symptom diary, noting down how often the attacks happen, any triggers, how long they last, how severe they are and where in your face is affected. This can help your health professionals identify the cause.
If your pain feels like it might be associated with one or more of your teeth, then it's worth visiting the dentist first. You may want to mention that you have MS, and trigeminal neuralgia may be a possibility. If the dentist cannot find anything wrong with your teeth or suggests major dental treatments, such as an extraction or root canal, it's worth exploring the possibility of trigeminal neuralgia before proceeding further.
If you think the pain could have another cause, like an ear infection, speak to your GP who can do a bit more investigation.
Although there is no cure for trigeminal neuralgia, there are treatments that can ease the pain and reduce its impact on your life. Medicines are usually offered first.
Like other forms of nerve pain, trigeminal neuralgia is not eased by common painkillers like paracetamol, aspirin or ibuprofen.
Your MS team or GP should offer a medicine called carbamazepine to begin with. This is the recommended first-line treatment for trigeminal neuralgia. Carbamazepine is commonly used to treat epilepsy, but research shows it can help with trigeminal neuralgia too. It's thought to work by interfering with the delivery of pain messages to the brain, reducing the amount of pain you feel.
You take carbamazepine several times a day, increasing the dose slowly over a few days or weeks until an effective dose is reached. If you need to stop carbamazepine for any reason, you’ll usually need to reduce the dose gradually.
Some people find that carbamazepine works very well at relieving pain initially, but with longer term use it becomes less effective.
If this medicine does not work well, causes too many side effects or the effects wear off, you may be referred to a pain specialist, neurologist or neurosurgeon to discuss other options that may help.
A specialist may recommend other medicines that are used for nerve pain, such as oxcarbazepine, lamotrigine, gabapentin or pregabalin. They may recommend baclofen which can relax your muscles and help ease the pain.
Botulinum toxin (Botox) injections may also be an option. While botulinum toxin is best known for its use in cosmetic procedures, it can also help manage some MS symptoms. In trigeminal neuralgia, it’s thought that botulinum toxin injections may help relieve pain when used in painful areas on the face. It’s thought to work by blocking pain messages. This treatment has to be delivered by a neurologist with experience in facial pain management.
If the medicines discussed above do not control your pain well enough, your specialist may suggest surgical options or radiotherapy.
There are a number of surgical procedures to treat trigeminal neuralgia. Your neurosurgical team should explain what type of procedure may be suitable for you, and the possible risks and benefits of any surgery. This will vary from person to person.
Here we briefly explain the different surgical procedures. This information might help you prepare for your appointment with a neurosurgeon and help you think about what questions you could ask them.
There are several possible procedures that involve inserting a needle or thin tube through your cheek to stop pain signals travelling along the trigeminal nerve. These are called percutaneous procedures (percutaneous means through the skin). X-rays are used to help guide the needle or tube to the correct place.
The procedures are done while you are heavily sedated or under a general anaesthetic. Sedation is where you’re given medicine to make you feel drowsy and relaxed. You can usually go home the same day.
These treatments work by deliberately injuring the trigeminal nerve in a controlled way to disrupt the pain signals travelling along it.
They provide immediate pain relief and are very effective for the majority of people initially. However, the effect seems to reduce over time, usually over a few years. In some cases, the procedure may need to be repeated or a different one tried.
The most common side effect is varying levels of numbness. This often reduces over time, but in rare cases it can be permanent. This can affect all or part of the face. It can feel similar to when you've had an injection at the dentist.
If these procedures are repeated, your risk of developing anaesthesia dolorosa (painful numbness) increases. This is where you experience continuous pain in the numb area of your face. There are currently no treatments for this, but it is a very rare side effect.
Microvascular decompression is a major surgical procedure that may be used if trigeminal neuralgia is caused by a blood vessel pressing on the nerve. It is the gold standard surgical treatment for classical trigeminal neuralgia. The procedure is carried out under general anaesthetic by a neurosurgeon. A small part of your skull is removed behind the ear to relieve the pressure on the nerve and move the blood vessel away.
This procedure is very effective in people with classical trigeminal neuralgia and is considered the closest treatment to a cure. However in people MS, this procedure is not used routinely as facial pain in MS is usually caused by nerve damage rather than a blood vessel pushing on the nerve.
Your neurosurgeon would talk you through this procedure and support you in weighing up the risks and benefits before you decide if it’s something you want to go ahead with.
This is a type of radiotherapy rather than a surgical procedure. It's commonly used to treat small tumours but can also be used to treat trigeminal neuralgia.
A concentrated beam of radiation is used to damage the trigeminal nerve and stop the nerve from sending pain signals. It does not involve having an incision (cut) in your cheek. You will not need a general anaesthetic.
Stereotactic radiosurgery is delivered by specialist machines (Gamma Knife, CyberKnife or linear accelerator/LINAC). You'll usually have to lay down and have a special frame over your head to keep it still. Then the machine uses beams of radiation to damage the nerve.
It can take a few weeks for the procedure to take effect, but it can offer pain relief for several months or years. Like the percutaneous procedures discussed above, numbness on the face is a common side effect which can sometimes be permanent.
Research shows that stereotactic radiosurgery is effective in around 8 in every 10 people who have this procedure. Pain relief often reduces over time, usually a few years, so the procedure may be repeated.
The NHS website has more information on surgical procedures and radiotherapy for trigeminal neuralgia (NHS.UK).
If trigeminal neuralgia is impacting on essential activities, like eating, washing and cleaning your teeth, it might be useful to see an occupational therapist (OT) for support. An OT can suggest alternative ways of doing things or equipment that may help. They can also help if numbness in your face is causing problems after having one of the procedures discussed above.
If your pain interferes with, or is made worse by, biting or chewing, you may find that eating softer food or liquidising food helps. If you're losing weight because of difficulties with eating, speak to your GP and ask to be referred to a dietitian for support.
Living with persistent trigeminal neuralgia can affect your mental health. If you're noticing a change in your mood and you're feeling low, you may want to consider reaching out for support from a psychological therapy service.
These services offer therapies to help you develop coping strategies and change how you respond to pain. They may offer therapies such as counselling, cognitive behavioural therapy, mindfulness and acceptance and commitment therapy.
Your GP or MS team can refer you to your local service. Alternatively, if you live in England, you can self-refer. Find your local talking therapy service (NHS.UK)
Read more about psychological therapies
Alongside the treatment options discussed above, there are things you can do to manage facial pain yourself. This includes noticing what triggers your pain and, if you can, making changes to how you do daily activities. Complementary therapies, distracting yourself and relaxation techniques can be useful too.